

Journal of Clinical and Biomedical Sciences
DOI: 10.58739/jcbs/v16i1.25.227
Year: 2026, Volume: 16, Issue: 1, Pages: 21-28
Original Article
Nikhil P Hawal1*, Namratha Kulkarni2, Someswara G M1, Satish Dhamankar3
1Associate Professor, Department of Community Medicine, S. R. Patil Medical College, Badgandi, Badagandi Taluk, Bilagi, District, Bagalkot- 587116, Karnataka, India.
2Associate Professor, Department of Community Medicine, KAHERS’s agadguru Gangadhar Mahaswamigalu Moorsavirmath Medical College (JGMMMC), Hubballi, Karnataka, India.
3Professor, Department Of Obstetrics and Gynaecology, USM KLE International Medical Program and KLE Centenary Hospital, Yellur, Belagavi, India.
*Corresponding Author
Email: [email protected]
Received Date:08 May 2025, Accepted Date:29 July 2025, Published Date:31 March 2026
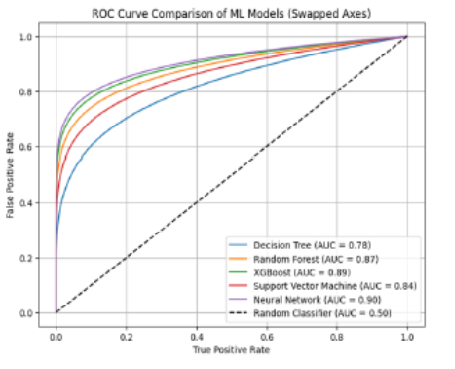
Low birth weight (LBW), defined as birth weight below 2,500 grams, remains a significant public health concern in India, affecting approximately 17.29% of infants according to NFHS-5 data. This study aimed to develop and evaluate artificial intelligence (AI) models for predicting LBW using maternal, socioeconomic, and antenatal care-related factors derived from NFHS-5. A dataset of 662 records was extracted following stringent inclusion criteria, with 530 records allocated for training and 132 for testing. Feature selection was conducted using recursive feature elimination, identifying 24 key maternal predictors, including maternal age, education, BMI, anemia status, antenatal visits, and socioeconomic status. The AutoGluon framework was utilized to build predictive models, incorporating ensemble methods such as CatBoost, LightGBM, Random Forest, Extra Trees, K-Nearest Neighbors, and Neural Networks. The best predictive model was the Neural Network, with an accuracy of 86%, sensitivity 82%, specificity 89%, and AUC-ROC of 0.90. XGBoost and Random Forest were not too far behind with AUC-ROC scores of 0.89 and 0.87 as well. Maternal education, hemoglobin levels and birth intervals were identified as the most relevant predictors of LBW in the analysis of the feature importance. This study highlights the effectiveness of predictive modelling using AI in the detection of different risk factors associated with Low Birth Weight (LBW) and demonstrates its implication in predicting women at high-risk and in administering targeted prevention interventions to prevent LBW. This indicates that machine learning models into maternal healthcare processes could be utilized to conduct better early risk assessment and ensure appropriate precautions are taken in a timely fashion. To enhance the clinical utility, future research should target on external validation and real-world implementation.
Keywords: Low Birth Weight (LBW), Machine Learning, Maternal Risk Factors, NFHS-5, Predictive Modeling, Neural Networks
1. International Institute for Population Sciences (IIPS) and ICF. <I>National Family Health Survey (NFHS-5), 2019-21</I>: India. Mumbai: IIPS; 2021. Available from: https://dhsprogram.com/pubs/pdf/FR375/FR375.pdf
2. Khan JR, Islam MM, Awan N. Prevalence and correlates of low birth weight in India: a systematic review and meta-analysis. <I>BMC Pregnancy Childbirth</I>. 2023;23:803. doi:10.1186/s12884-023-06128-w. Available from: https://bmcpregnancychildbirth.biomedcentral.com/articles/10.1186/s12884-023-06128-w
3. Ranjbar A, Montazeri F, Farashah MV, Mehrnoush V, Darsareh F, Roozbeh N. Machine learning-based approach for predicting low birth weight. BMC Pregnancy and Childbirth. 2023; 23 (1). Available from: https://doi.org/10.1186/s12884-023-06128-w
4. Kader M, Perera NKP. Socio-economic and nutritional determinants of low birth weight in India. North American Journal of Medical Sciences. 2014; 6 (7). Available from: https://doi.org/10.4103/1947-2714.136902
5. World Health Organization (WHO). <I>Global Nutrition Targets 2025: Low Birth Weight Policy Brief</I>. Geneva: WHO; 2014. Available from: https://www.who.int/publications/i/item/WHO-NMH-NHD-14.5
6. International Institute for Population Sciences (IIPS) and ICF. <I>National Family Health Survey (NFHS-4), 2015-16</I>: India. Mumbai: IIPS; 2017. Available from: https://dhsprogram.com/pubs/pdf/FR339/FR339.pdf
7. International Institute for Population Sciences (IIPS) and ICF. <I>National Family Health Survey (NFHS-3), 2005-06</I>: India. Mumbai: IIPS; 2007. Available from: https://dhsprogram.com/pubs/pdf/FRIND3/FRIND3-Vol1AndVol2.pdf
8. United Nations Children’s Fund (UNICEF) and World Health Organization (WHO). <I>Low Birthweight: Country, Regional and Global Estimates</I>. New York: UNICEF; 2004. Available from: https://www.unicef.org/reports/low-birthweight
9. Kumar A, Singh T, Basu S, Pandey S, Bhargava V. Outcome of low birth weight neonates in a tertiary care hospital in North India. <I>Journal of Clinical Neonatology</I>. 2013; 2 (4). Available from: https://doi.org/10.4103/2249-4847.123080
10. Riley RD, Ensor J, Snell KI, Harrell Jr FE, Martin GP, Reitsma JB<I>et al</I>. Calculating the sample size required for developing a clinical prediction model. BMJ. 2020; 368 Available from: https://doi.org/10.1136/bmj.m441
11. Erickson N, Mueller J, Shirkov A, Zhang H, Larroy P, Li M, <I>et al</I>. AutoGluon-Tabular: Robust and Accurate AutoML for Structured Data. <I>arXiv preprint</I> arXiv:2003.06505. 2020 Mar 13.
12. Khatun S, Rahman M. Socio-economic determinants of low birth weight in Bangladesh: A multivariate approach. Bangladesh Medical Research Council Bulletin. 1970; 34 (3). Available from: https://doi.org/10.3329/bmrcb.v34i3.1857
13. Kumar M, Tripathi S, Kumar J, <I>et al</I>. Predictors of low birth weight in North India: An institutional based study. <I>Indian Journal of Community Medicine</I>. 2020;45(3):277-282.
14. Ahankari A, Myles P, Fogarty A, <I>et al</I>. Maternal hemoglobin status and pregnancy outcomes: A systematic review and meta-analysis. <I>Public Health Nutrition</I>. 2019;15(2):123-130.
15. Black RE, Victora CG, Walker SP, Bhutta ZA, Christian P, de Onis M<I>et al</I>. Maternal and child undernutrition and overweight in low-income and middle-income countries. The Lancet. 2013; 382 (9890). Available from: https://doi.org/10.1016/s0140-6736(13)60937-x
16. Kader M, Perera NK. Socio-economic and nutritional determinants of low birth weight in India. North American Journal of Medical Sciences. 2014; 6 (7). Available from: https://doi.org/10.4103/1947-2714.136902
17. Singh S, Shekhar C, Acharya R, <I>et al</I>. The incidence of low birth weight in India: A case study using NFHS-4 data. <I>BMC Pregnancy and Childbirth</I>. 2019;19(1):377.
18. Patel R, Gupta A, Chauhan S, Bansod DW. Effects of sanitation practices on adverse pregnancy outcomes in India: a conducive finding from recent Indian demographic health survey. BMC Pregnancy and Childbirth. 2019; 19 (1). Available from: https://doi.org/10.1186/s12884-019-2528-8
19. Anand K, Garg BS. A Study of Factors Affecting LEW. Indian Journal of Community Medicine. 2000; 25 (2). Available from: https://doi.org/10.4103/0970-0218.34086
20. Silvestrin S, Silva CH, Hirakata VN, Goldani AAS, Silveira PP, Goldani MZ. Maternal education level and low birth weight: a meta-analysis. Jornal de Pediatria. 2013; 89 (4). Available from: https://doi.org/10.1016/j.jped.2013.01.003
21. Agarwal N, Reddaiah VP. Factors affecting birth weight in a sub-urban community: A study in a secondary level hospital in Delhi. <I>Indian Journal of Pediatrics</I>. 2018;72(8):745-750.
22. Muhammed T, Meharban S, Tabassum R. Machine learning techniques for predicting low birth weight based on maternal characteristics: A comparative study. <I>Proceedings of the International Conference on Smart Systems and Inventive Technology</I>. 2020:762-767.
23. Koullali B, Oudijk MA, Nijman TA, Mol BWJ, Pajkrt E. Risk assessment and management to prevent preterm birth. Seminars in Fetal and Neonatal Medicine. 2016; 21 (2). Available from: https://doi.org/10.1016/j.siny.2016.01.005
24. Tejal P, Neeta M, Prashant B. Application of data mining techniques for prediction of low birth weight - A decision support system. <I>International Journal of Computer Sciences and Engineering</I>. 2017;5(3):156-162.
25. Sharma D, Shastri S, Sharma P. Intrauterine Growth Restriction: Antenatal and Postnatal Aspects. Clinical Medicine Insights: Pediatrics. 2016; 10 Available from: https://doi.org/10.4137/cmped.s40070
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Published By Sri Devaraj Urs Academy of Higher Education, Kolar, Karnataka
Subscribe now for latest articles and news.